Not all cancer cells are equal. Tumour recurrence often depends on a few active cells. Researchers Miao-Ping Chien and Daan Brinks can recognise and target those cells.
Miao-Ping Chien and Daan Brinks aline biology and physics in the battle against cancer. (Foto: Eramus MC)
Chien and Brinks are role models for the Convergence collaboration between the Delft University of Technology and the Erasmus Medical Centre. In Convergence, researchers work on the simultaneous development of technology and healthcare. She (Dr Miao-Ping Chien) has a broad background in the biology of cancer cells, biochemistry and biophysics. He (Dr Daan Brinks) adds a combination of neuroscience and physics. They both followed an intensive training in multidisciplinary work at Harvard University, where they met each other and where they stayed until 2017. Then they moved together to the Netherlands, each setting up their own lab: the MP Chien Lab at the Erasmus MC and the Brinks Lab at TU Delft.
Their multidisciplinary approach, and the work of more than 30 staff and students, has since led to a miraculously advanced microscope that can pick out a few of the most active cells from a sample of 20,000 to 30,000. They recently published about it in Nature Biomedical Engineering (17 March 2022), are offering the technology to practitioners at Erasmus MC, and are working on a spin-off under the name UFO Biosciences.


Artist’s impression of the UFO-microscope. (Illustration: Still from video)
The UFO (Ultra-wide Field of view Optical) microscope is about the size of an old-fashioned desktop computer and, according to Miao-Ping Chien, basically consists of “a combination of many lenses, mirrors, lasers and filters”. The microscope is unique in the sense that it allows the study of many cells simultaneously, Brinks explains: “This is done with sufficient resolution in space and time that allows you to follow individual cells and do that for a very large number of cells at the same time.”
Cells in motion
Not all cancer cells are the same, Chien explains. “Over the past decade, people have started to realise that a small proportion of cancer cells are responsible for metastasis and resistance to therapies.” When she set up her lab at Erasmus MC in 2017, it was with the intention of developing a technique that could image precisely those most dangerous cells. Now, scarcely five years later, the UFO has landed.
“Under the microscope we look at how cancer cells move. Most cells hardly move at all, but there are always a few that show a more directed movement. We know from in-vivo studies that it is these moving cells that cause metastasis,” Chien continues.
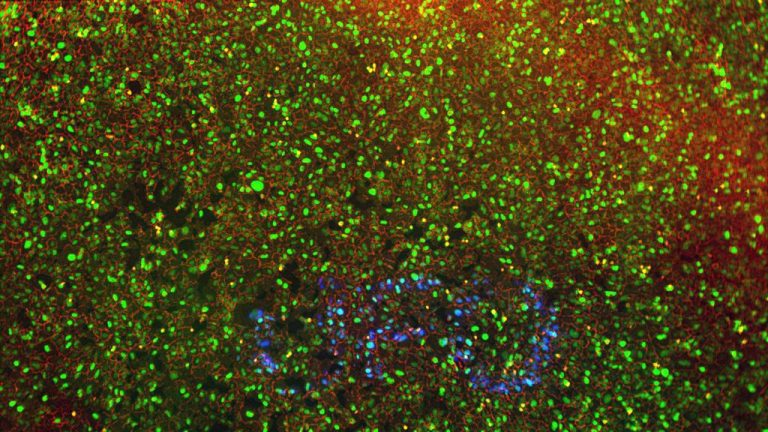

The UFO-microscope shows the most active cancer cells in a different colour. (Photo: UFO Biosciences)
Being able to pinpoint the most aggressive cancer cells within an environment of tens of thousands of cells is already quite an achievement, but how do you isolate them? Chien has come up with a master plan to do just that. She ensures that all cells contain a photo-activatable dye. The dye in the cells that display directed movement are activated with a light beam. The colour then isolates the most dangerous cells from the rest.
De animatie toont de identificatie van agressieve tumorcellen.
Under the bonnet
For about 10 years now, it has been possible to read the hereditary material of a single cell. Many researchers prefer the working copy RNA to the full library of DNA. A cell makes a functional copy of the DNA (genes) called RNA. This serves as a recipe for assembling proteins from amino acids. “From the RNA we can see which genes are active in aggressive tumour cells and what biochemical signals and reactions the cell uses,” explains Chien.
From single cell sequencing, there are two possible follow-up routes. The first is that of biomarkers – specific RNA sequences like fingerprints from which an active tumour cell can be recognised. Doctors can use these to see whether a tumour is causing metastases. The second pathway is that of pharmaceuticals. When researchers know the exact biochemical signals and reactions these cells use, they can look for medicines to block them.
Clinical relevance
Over the past two years, researchers at the Chien Lab have worked on two types of tumours from which they have derived a set of biomarkers or genetic signatures. Soon, they will investigate whether the biomarkers predict metastases in a larger group of 50 – 100 patients as well.
“We would like to see this technique become an accepted diagnostic tool in hospitals,” says Brinks. “Cells from a biopsy go in, and it gives advice on the most suitable treatment for this patient. But we still have much to do before we can achieve this – scientifically as well as in the development of the microscope, of which there now are only two. For this, we need to collaborate with researchers and therapists who are interested in our data, and with pharmaceutical companies who are interested in the biomarkers and in the potential for drug development. We have already started those conversations, and the response so far has been hopeful.”
“In the beginning, the UFO microscope was primarily a research tool,” says Chien looking back, “but the other side of my heart was crying out for more, longing to develop something that could really improve the clinical treatment of cancer patients. That has become our shared dream.”
- More about the Convergence programme
- Also read Spotlight on aggressive cancer cells (Erasmus MC)
Do you have a question or comment about this article?
j.w.wassink@tudelft.nl


Comments are closed.