Medical staff at the LUMC are interested in working with TU Delft to see how hospitals can reduce their ecological footprint. ‘One snip and the scissor is thrown away.’
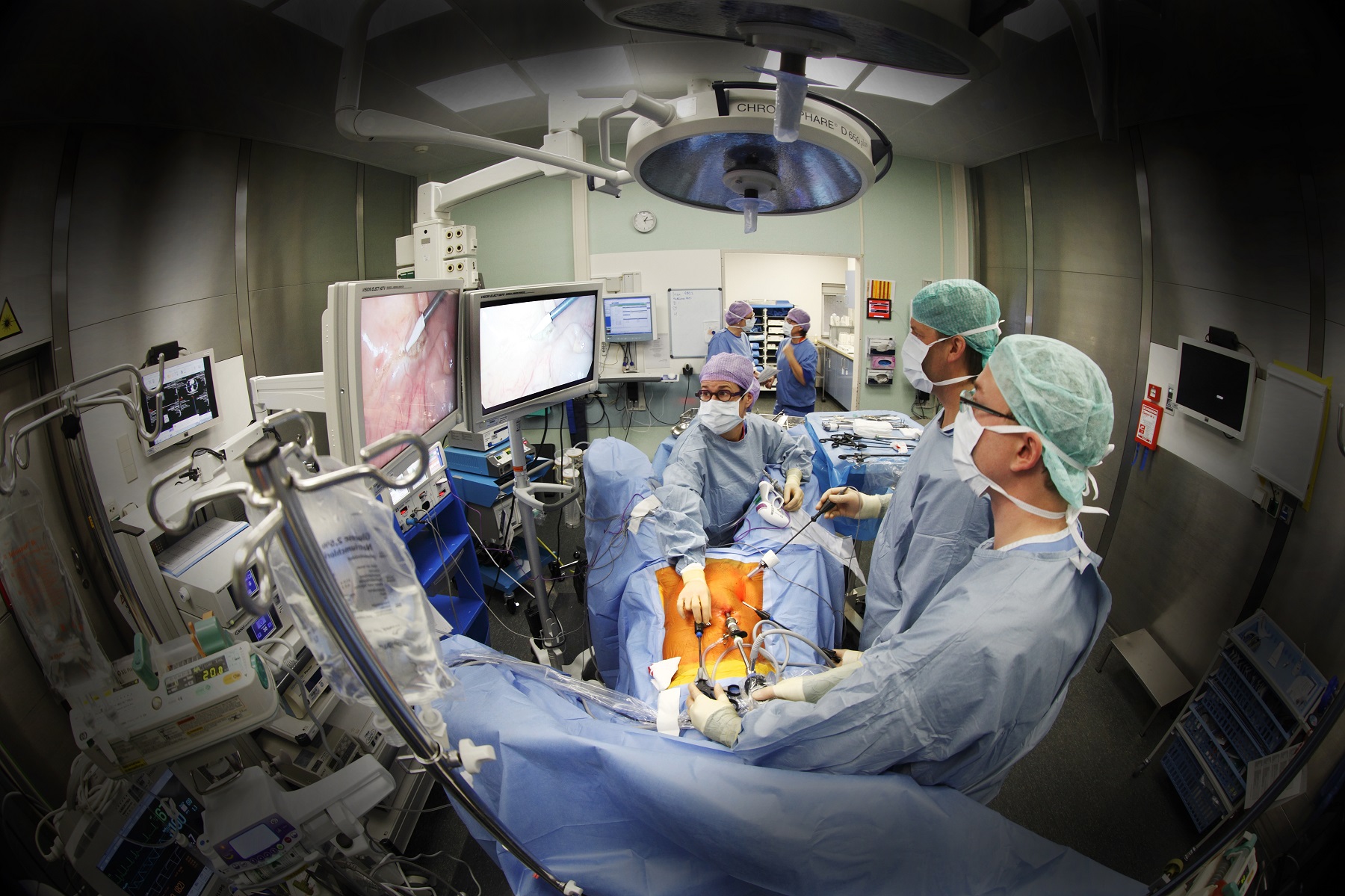
Among the things that worry the doctors is the enormous quantity of disposable products used in operation rooms that create mountains of waste. (Photo: Hans Stakelbeek)
If you think about CO2 emissions, you probably think about heavy industry and transport. But hospitals are huge polluters, says a group of medical staff at the Leiden University Medical Centre (LUMC). Hospitals account for 2% to 5% percent of all CO2 emissions in western countries they say, quoting an as yet unpublished literature study. They want to see how the ecological footprint of operation rooms can be reduced.
One of the initiators of the collaboration is the gynaecologist Frank Willem Jansen who is also associated with the Biomechanical Engineering Department at TU Delft. “The Netherlands wants to reduce its CO2 emissions by 95% in 2050 from 1990 levels,” he says. “For the healthcare sector, this goal was included in the Greendeal 2.0 ‘Duurzame zorg voor een gezonde toekomst’ (sustainable care for a healthy future) in 2018. Great, a plan like this, but in the meantime, little is being done.”
Disposable products
“The healthcare sector contributes to CO2 emissions, exploitation of resources and pollution of the earth and is thus partly responsible for the negative effects on human health,” he summarises. “We all see these effects. We suddenly see mosquitos here that can carry malaria. There are parakeets flying around. Pretty birds you may think, but they do not belong here.”
On the agenda is the ecological footprint of all the materials that are used in ORs and how these can be reduced. Among the things that worry the doctors is the enormous quantity of disposable products used in operation rooms (ORs) that create mountains of waste. On 1 July, they will meet with TU Delft engineers in cooperation with the TU Delft Health Initiative. On the agenda is the ecological footprint of all the materials that are used in ORs and how these can be reduced. They believe that TU Delft engineers should be well placed to help. Some TU Delft students are already working on a preliminary study.
Anne van der Eijk, a biomedical engineering alumni, is involved in the project. She is the manager of the OR centre and the sterilisation department of the LUMC. “My job is to support healthcare providers so that they can give good and safe care. That is top of the list. But I also see it as my job to reduce the CO2 footprint. We use so very many disposable items. If we could buy more sustainable materials and reusable products we would be able to reduce that CO2 footprint. Even cleaning and sterilising surgical instruments could probably be done in a much more environmentally friendly way.”
‘Operation overalls are also only used once’
Co-initiator Hans Friedericy painfully watches how most of the materials used in ORs are thrown away after one single use. “We are working more and more with disposables. One scissor, one snip and it ends up in the rubbish bin. Operation overalls are also only used once. These overalls used to be washed and reused the next day.”
This trend started 20 years ago, Friedericy continues. “Disposable products were considered cleaner and cheaper as they did not need to go through the sterilisation process. That may have been the case before, but we wonder if it is still the case now. Sterilisation machines have become much more efficient. They use less water and less electricity. On top of that, the residual heat is used to heat the hospital.”
On the agenda is also the energy guzzling air treatment in ORs. The ventilation systems in the 20 ORs at LUMC run 24/7. The air in an OR must be completely refreshed every two or three minutes. New air has to reach the right temperature and the right humidity. But not all the ORs are used at night.
Anaesthesiologists can dramatically reduce the CO2 footprint in their daily practice
Friedericy says that “We should look at the protocols again. The energy consumption to continually refresh the air is extremely high. In the USA they turn off three-quarters of the machines at night as the ORs are not in use anyway. Should there be a disaster – a big accident or attack – and you suddenly need full capacity, the ORs are ready for use in 20 or 30 minutes. With a bit of luck the first surgeons who are woken up will be at the hospital around then.”
The third point of the medical staff’s plan is the anaesthesia. Anaesthesiologists can dramatically reduce the CO2 footprint in their daily practice by opting for intravenous anaesthesia instead of inhalation anaesthesia. In the former, the hypnotics are shot straight into the bloodstream while, in the latter, the medicine is given in the inhalation air.
In contrast to intravenous anaesthetics, inhalation anaesthetics have a greenhouse gas effect. After breathing, inhalation anaesthetics are barely metabolised in the body and are emitted unchanged into the atmosphere during exhalation. The infrared absorbing properties in the atmosphere make these, and other fluorinated gases such as chlorofluorocarbons (CFCs), a greenhouse gas. “In 2014, the worldwide emission of inhalation anaesthetics was equivalent to the annual emissions of about 650,000 private vehicles,” says Friedericy.
‘This would be a good subject for research for TU Delft engineers’
Friedericy believes that anaesthesiologists are adept at both techniques and there is usually no reason to choose inhalation anaesthetics. “I opt for inhalation anaesthetics if I have to anaesthetise babies because it is not pleasant to inject little baby arms. And I know that some anaesthesiologists use inhalation anaesthetics for obese patients because less of the anaesthetics is absorbed in the fat tissues.” But he calls these exceptions as most patients do well with intravenous anaesthetics. “And it should be technically possible to collect the inhalation anaesthetics after use so that they do not enter the atmosphere and can even be reused. This would be a good subject for research for TU Delft engineers.”
Do you have a question or comment about this article?
tomas.vandijk@tudelft.nl

Comments are closed.