Clinical breast examination is one of the ways to detect breast disease. However, medical students don’t properly learn palpation skills. New breast models should change that.
Dr Daisy Veitch on her visit to Delft. (Photo: Jos Wassink)
There is a problem in medical training with learning to feel for anomalies in breast tissue, says Dr Daisy Veitch who received her PhD for the development of a tactile accurate breast model. “Traditionally,” she explains, “breast surgeons observe students examining a patient. They then mark them according to criteria such as: did they cover all the areas of the breast, did they use the appropriate technique, did they press hard enough, did they introduce themselves to the patient?”
How are students supposed to distinguish a cyst from a tumour by touch?
But in terms of the purpose of the examination, being able to pick out the person with breast cancer from a test group, students perform no better than chance. Scary as the implications may be, it’s the best that current medical education has to offer. Under test conditions in a medical school, the patient is always an actor and there are no clinical findings. There is nothing to find. So, how are students supposed to learn what a lump feels like or how to distinguish a cyst from a tumour by touch?
Palpation, the examination of a patient by touch, is part of clinical breast examinations (CBE), together with oral history and visual inspection. CBE is one of three components of the so-called Triple Test for breast cancer, the others being radiological imaging and biopsy.
Meet Daisy Veitch, managing director of SHARP Dummies, a producer of soft manikins for the fashion industry and, recently, for medical training. For her, everything came together at the Human Factors Conference in Sydney. Professor Harry Owen (Flinders University) had pointed out to her that there were no realistic manikins for training CBE and no test objects for testing palpation skills. She received the best paper award from Human Factors Society of Australia whereProfessor Richard Goossens of TU Delft was the keynote speaker, and she was already acquainted with Dr Johan Molenbroek of the TU Delft Faculty of Industrial Design Engineering (IDE). And so, there and then, the idea was born: Daisy Veitch, with all her experience in human modelling with soft materials, was to develop model breasts for clinical training as a PhD project.
She had wide support from the community of breast surgeons. “I went into surgery with Melissa (Dr Bochner of the Royal Adelaide Hospital, ed.),” Veitch later wrote in an article for the Asian Hospital and Healthcare Management journal. “The patient, who had breast cancer, was having a mastectomy. The surgeons took the removed breast and gave it to me on a tray so I was able to feel it and examine it and build a comparable breast model right next to it. That first model was relatively easy to develop. From there, getting other variations like thickness and softness, and understanding what causes these variations was much more difficult.”


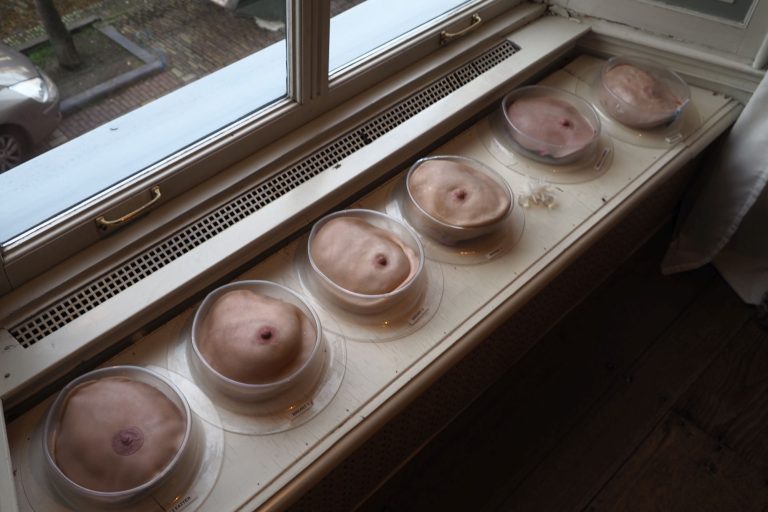
Veitch has developed six breast models of different lumpiness, thickness and softness. At her PhD defence, she even passed a model on a plate to the audience and encouraged them to examine it thoroughly. Initial prudishness soon gave way to fascination and wonder of the object under one’s fingers. Clearly, it’s not that easy to discover hidden features in the soft and yet firm mass.
It turns out that breast models are used in medical training, and they’re also available for self-examination. What is the difference between the existing models and the breast models that Veitch developed?
Veitch explains that “there are three differences. The first is that the existing models on the market don’t represent a range of anatomical variation. People vary in lots of different ways and some ways are important for teaching breast examination. It doesn’t matter if the colour of the breast model varies, but we believe that the softness or hardness of a breast matters. The second thing is that the nodularity or lumpiness in the breast matters. It used to be that all models were too simple. The models didn’t feel realistic in any way but their hardness made them extremely durable. Softer models won’t last as long. Most of the old models also do not have any pathology, and the ones that do have a degree of pathology are simplistic and the anomalies are very easy to find. And the third thing is that there is no testing component for students to learn palpation skills. In medical schools, if students learn using models, they may use the very same models during their exams. This means that they are only going through the motions of palpation as they already know where the breast lumps are. There are no specialised test objects that students haven’t seen before to really examine their palpation skills.”
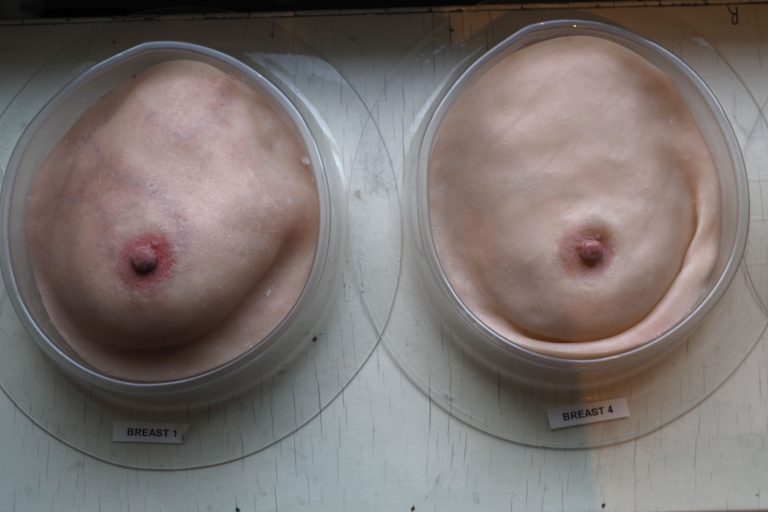

How do you know your models are realistic?
“We gave the models to five breast surgeons. The surgeons took them to a clinic. The doctors palpated both patients and the models and filled in a questionnaire at the end of each examination. It turns out that in 82% of the time, our models were similar to the patient. We were absolutely thrilled with the results from these experts. We also know that we need to make one more model: a very soft breast model. At the moment we have six variations of models which are useful in teaching. We would like to add a seventh very soft model.”


Did you include various pathologies as well?
“We made different objects according to 2D visual ultrasound images. I didn’t know what the shapes were, since we only had a slice sample. I was able to look at slices from different angles and create a 3D image in my mind. A cyst is easy because it’s round and looks like a disc. I made the shapes in different kinds of stiffness and I took them to Dr Melissa Bochner. We put them under different layers of fat and skin under different circumstances. I had inserted and marked various objects in the shapes and she reported if they were similar or not similar to real anomalies. We determined the best materials by a process of elimination. I made lots of test objects and she either selected the best ones or advised me on improving others. So it was basically iterative design.”


You also developed a flat model called the ‘tactile landscape’ with variations in depth, tissues, normal anatomical features and pathologies, all hidden. What is its purpose?
“Initially the idea was to test the breast models, but we found that we couldn’t really test them.. What we could test was the tactile landscape and the proctoring – the traditional way of teaching palpation skills. What makes our work so innovative is that we are now introducing a way to really test the comprehension component of clinical breast examination, which is the palpation skills.”
You’ve successfully finished your PhD. What is the next step?
“We want to develop this further. We need to get some funding at this stage. We need to develop a teaching package around the breast models, and for the tactile landscape we need to get a validated test protocol. Professor Jenny Dankelman (3mE) obtained one for a liver palpation model so she has already forged that path. I had a meeting with her and I hope that a student will take on the challenge of further development so that we can make the tactile landscape ready to sell.”
Where do you want to launch the tactile landscape as a medical training tool?
“I think we would launch it in Europe because the network of people here offers a channel to market. It will be so much easier the second time around I think. I think the tactile landscape would be absolutely relevant to other high income countries, in particular Australia and the USA. I think the easiest way forward would be to work on the test object, which is the tactile landscape. It would be simpler to produce, faster to bring to market and the benefits are very clear. And it also doesn’t require any kind of delays like adding a teaching package. So it’s closer to market, closer to commercialisation. If the tactile landscape generates an income, this would allow us to further fund the development of the breast models and turn them into a commercial product as well. So we need to bootstrap it to get the breast models going.”

-
Daisy Ellen Veitch, A Tactile Correct (Biofidelic) Teaching Model for Training Medical Staff to Diagnose Breast Cancer, PhD supervisors Prof. Richard Goossens and Dr Johan Molenbroek (IDE), 9 December 2019.
Selected articles to download:
Development and Pilot of Tactile Landscape
Evaluation of Clinical Breast Examination
Do you have a question or comment about this article?
j.w.wassink@tudelft.nl


Comments are closed.